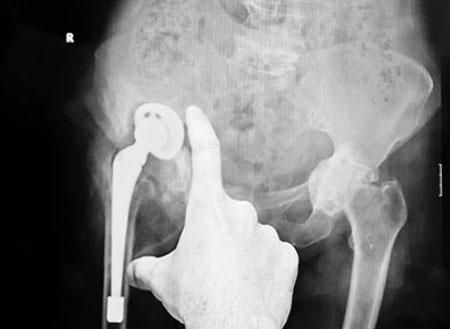
Knock knock. “Hello, I am here to take you for x-rays.” Has this ever been your experience at a doctor’s appointment? Have you ever been exasperated because you feel like you have had four sets of wrist x-rays over the last few months? Have you ever questioned whether or not the x-rays are necessary? Have you ever walked down the clinic hallway wearing the most fashionable blue shorts or over-sized gown known to mankind? Here at Orthopaedic Associates of Wisconsin, the skeleton is our specialty. Consequently, we take a lot of x-rays and keep our eight radiologic technologists quite busy. Luckily, I caught them on a day that wasn’t so busy and took some time to get answers to some of the most frequently asked questions regarding the world of x-ray.
The process of x-raying a body part has morphed significantly over the years. As you may have guessed, it’s all digital now. Just like you no longer have to take your camera film to a drug store to be developed, you no longer have to wait for films of x-rays to dry to be read by a radiologist or doctor on a view box. At our clinic here in Pewaukee, as the x-rays are taken, the images are saved onto the computer, and by the time you return to your exam room, typically your doctor is opening up the link to be able to see them on his computer as well.
X-rays are vital to proper care and treatment of musculoskeletal injuries. We are often asked why we have to get images if no fracture is expected. Bone fractures are only a small aspect of what we are trying to assess. In our adolescent patients, we are looking for growth plate closure. We are looking to see if any bone spurs have developed due to repetitive trauma that may be causing pain in an area. When people come in with complaints of a mass or cyst somewhere on their body, we use x-rays to determine the depth of the cyst as they can be like icebergs that appear small, but are expansive under the skin. We have identified cancerous masses that require further work-up. We can see the extent of degenerative joint disease or arthritis to determine if someone is a candidate for a total joint replacement. We can see bone spurring that may be impinging soft tissues like muscles or tendons. Sometimes injuries to soft tissues can pull a piece of bone away from the main structure, and that will appear on an x-ray.
If a fracture is identified, often times it requires continual monitoring while it heals. Sometimes fractures are unstable and can be aligned anatomically at your first appointment, but a follow-up set of x-rays shows that the fracture has fallen out of alignment, and now you are a surgical candidate. The nifty software our providers use for evaluating fractures has tools for measuring the displacement or angulation of a fracture so they know exactly how far out of place a fracture may be, which helps them with surgical planning. Similar tools such as Ortho View also allow our board-certified surgeons to determine what size prosthesis a total joint replacement patient needs.
Patients are often concerned about their radiation exposure during a routine series of x-rays. I asked my x-ray friends for some comparisons, and here they are. You could have 500 chest x-rays taken before you reach the annual limit of what is deemed safe by the United States Nuclear Regulatory Commission for a nuclear worker. That same x-ray is only minimally more exposure than what you receive taking a flight across the Atlantic Ocean - one way. That doesn’t include the flight back home again. Even if you sustain a fracture of your ankle and have three images taken of the area every month for three months while you heal, the level of radiation exposure is still minimal.
This blog is written by one of our very own-Morgan. She is a certified athletic trainer working as a medical assistant with our providers each and every day in our clinic. She obtained a bachelor's degree in athletic training from Carroll University in Waukesha and a master's degree in Kinesiology from Michigan State University. She is excited to bring you updates and information about the happenings at OAW.