Orthopedic News & Updates
Explore the latest news from our practice, including expert tips, new treatments, provider updates, community events, and patient success stories.
ARTICLES & PRESS RELEASES

Cold Weather and Joint Health: How to Keep Moving Through the Bitter Cold
Winter arthritis pain is common in cold climates. Learn how cold weather affects joints and when to seek orthopedic care this winter.

We Accept UnitedHealthcare: Here for Your Orthopedic Needs
If you’ve been following the news, you may have heard that Ascension Wisconsin no longer accepts UnitedHealthcare insurance. For many patients, this sudden change has

Pain Awareness Month: How Orthopaedic Care Can Change Lives
Each September, Pain Awareness Month shines a spotlight on a challenge that millions of Americans face every day – chronic pain. At Orthopaedic Associates of

Orthopaedic Associates of Wisconsin Welcomes Shoulder and Elbow Specialist Derek Damrow, MD
Orthopaedic Associates of Wisconsin is excited to welcome Derek Damrow, MD, to our team of fellowship-trained orthopedic surgeons.

Youth Sports Are Back: Injury Prevention Tips
With the return of youth sports, families are thrilled to see their kids back on the field, court, and track. But as activity ramps up,
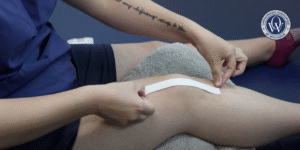
Boosting Surgical Recovery with Advanced Collagen Therapy
Healing after surgery is more than just waiting—it’s about equipping your body with the best tools for recovery. At Orthopaedic Associates of Wisconsin, we proudly introduce collagen-based dressing therapy, designed to enhance healing following hip, knee, cervical, or lumbar spine procedures.

Orthopaedic Associates of Wisconsin Breaks Ground on New Johnson Creek Facility
On July 7, 2025, Orthopaedic Associates of Wisconsin officially broke ground on a new 46,000‑square‑foot orthopedic clinic and outpatient surgery center at the intersection of Hartwig Boulevard and North Watertown Street in Johnson Creek, WI

Brace Fitting at Orthopaedic Associates of Wisconsin | What to Expect
At the Orthopaedic Associates of Wisconsin Bracing and Medical Equipment Department, your brace fitting is a personalized experience tailored to your diagnosis, symptoms, lifestyle, and goals.

Did You Know? The Incredible Benefits of Physical Therapy
When most people think of physical therapy, they often associate it with injury recovery. But did you know that physical therapy offers so much more?

A Comprehensive Approach to Spine Care with Dr. Mike Nolte
At the heart of our Spine Center is a team of providers with years of specialized training—from physical and occupational therapists to physiatrists, interventional radiologists, and surgeons. Our collaborative approach ensures that each patient receives the most comprehensive spine care available in Wisconsin. We integrate the newest and best technologies to provide complete care, all under one roof.

The Key to a Healthy Heart: Lifestyle Choices That Make a Difference
A healthy heart is the foundation of overall well-being. While genetics play a role in heart health, the lifestyle choices we make every day have

Celebrating National Athletic Training Month: The Vital Role of Athletic Trainers at OAW
March is National Athletic Training Month, a time to recognize the dedicated professionals who play a crucial role in injury prevention, treatment, and rehabilitation. While many
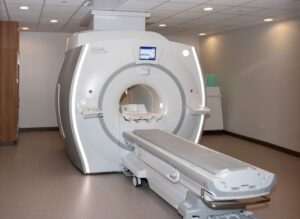
Understanding Your MRI: What to Expect and How to Prepare
At Orthopaedic Associates of Wisconsin, our advanced MRI technology delivers fast, detailed imaging in a comfortable environment—helping your care team diagnose and treat injuries with precision. With expert staff and streamlined scheduling, we make your imaging experience as easy as possible.
PHYSiCIAN'S VIDEOS
Get to know our orthopedic specialists through our physician video series. Each video offers a glimpse into the doctor’s background, areas of expertise, and personal approach to patient care. Whether you’re exploring your treatment options or meeting your provider for the first time, these videos help you connect with our physicians and better understand their commitment to helping you move without limits.
PHYSICAN PROFILES

2:02

1:26

1:37

1:26

2:14

2:16

2:21

1:35

2:06

1:52

1:49

2:04

1:59

2:18

2:28

1:54

2:04

2:46

2:00

2:10

1:58

2:22

1:53
TESTIMONIALS
Hear directly from our patients as they share their journeys to recovery with Orthopaedic Associates of Wisconsin. Our video testimonials highlight real experiences—from injury and treatment to life after surgery—showcasing the compassionate care and expert treatment that helped them return to their loved activities. These stories reflect the trust our community places in us and the impact of personalized, high-quality orthopedic care.
PATIENT TESTIMONIALS

1:57

2:17

1:37

2:41


